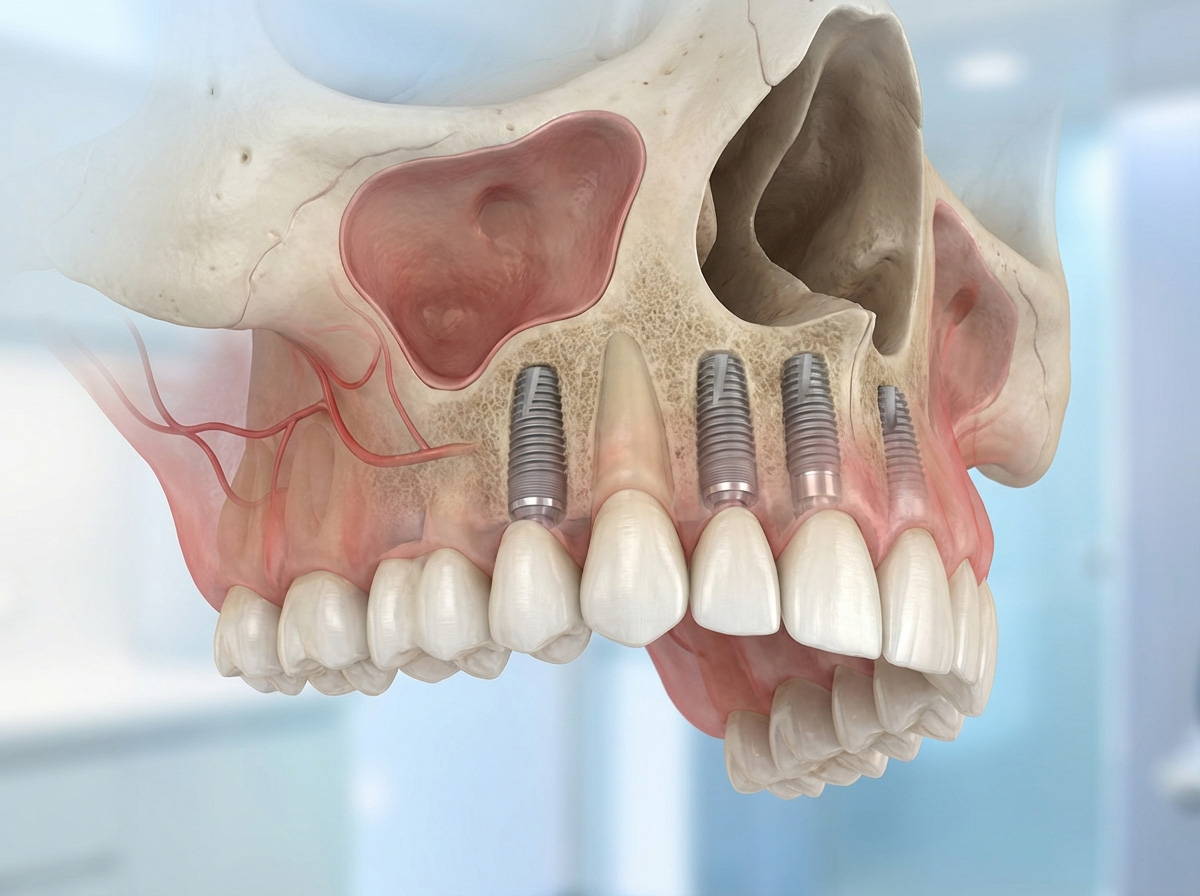
Upper jaw implant treatment offers a highly aesthetic, stable and functional solution for patients who have experienced tooth loss, bone resorption, or dissatisfaction with removable prostheses. With today’s digital dentistry technologies, implant placement in the maxilla has become significantly more predictable, minimally invasive and comfortable. This guide explains everything you need to know about upper jaw implants—from candidacy and treatment stages to bone grafting, sinus lifting, long-term success, and cost variables.
Maxillary Anatomy and Why It Matters in Implant Dentistry
The upper jaw (maxilla) has a naturally softer, more porous bone structure compared to the lower jaw. This makes anatomical evaluation crucial, especially in areas located close to the maxillary sinuses.
Because the bone density is lower, implant placement in the upper jaw requires precise planning. When bone height is insufficient, sinus lifting or bone grafting is performed to create a stable foundation for long-term implant success. These preparatory steps significantly improve the osseointegration rate and overall durability of the implants.
Who Is a Suitable Candidate for Upper Jaw Implants?
Upper jaw implants are ideal for a wide range of patients—from those missing a single tooth to individuals with full edentulism. Candidacy is determined by evaluating bone density, oral health, medical history and hygiene habits.
Suitable candidates include:
• Individuals with long-standing tooth loss in the upper jaw
• Patients experiencing bone resorption due to missing teeth
• Those dissatisfied with conventional bridges or removable dentures
• Patients who desire a permanent, natural-looking solution
• Individuals medically suitable for implant surgery
Since the upper jaw plays a major role in esthetics, proper implant angulation and positioning are essential to achieve both functional and cosmetic excellence.
Pre-Treatment Planning: The Stage That Determines 70% of Success
Successful upper jaw implant treatment depends heavily on detailed planning. With modern tools such as 3D CBCT scans, digital impressions and facial scanning, the ideal implant placement can be determined even before surgery begins.
During the planning stage:
• Bone height, width and density are measured
• The position and size of the sinus cavities are assessed
• Implant length, diameter and angulation are determined
• Aesthetic needs and smile design goals are analyzed
This ensures minimally invasive surgery, shortened duration, and a predictable healing process.
How the Upper Jaw Implant Procedure Works
Although each patient’s situation varies, the treatment typically progresses through the following stages:
1. Clinical Examination & 3D Imaging
The dentist evaluates bone quantity and quality using advanced radiographic imaging.
2. Surgical Preparations (Sinus Lift or Bone Grafting if Needed)
If bone structure is inadequate, regenerative procedures are performed to create sufficient support for the implant.
3. Implant Placement
Performed under local anesthesia, the implant is positioned into the bone with no discomfort. The surgical phase often takes 15–20 minutes per implant.
4. Osseointegration Period
The implant fuses with the bone within 2–4 months.
In the upper jaw, this period may be slightly longer than the lower jaw.
5. Restorative Phase (Temporary or Permanent Teeth)
Once healing is complete, abutments and final crowns are placed—harmonizing with the patient’s smile and facial proportions.
This structured workflow ensures both durability and natural-looking results.
Bone Loss in the Upper Jaw & The Role of Sinus Lifting
One of the most common challenges in upper jaw implantology is bone loss due to long-term tooth absence. When bone height reduces, the sinus cavity tends to expand downward, leaving insufficient space for implant placement.
In such cases, sinus lifting becomes essential. The sinus membrane is gently elevated, and bone graft material is added underneath. This creates the required bone volume for proper implant anchorage.
The procedure significantly enhances the long-term success rate of upper jaw implants.
Zygomatic Implants: A Lifeline for Severe Bone Loss
Some patients experience such advanced bone resorption that conventional implants are no longer feasible. For these complex cases, zygomatic implants—anchored into the cheekbone (zygoma)—provide a powerful alternative.
They are ideal for:
• Patients with extreme maxillary bone loss
• Individuals who previously experienced implant failure
• Patients unsuitable for grafting procedures
• Those seeking immediate fixed-teeth solutions
Zygomatic implants allow many patients to receive same-day, fixed prosthetic teeth and avoid extensive bone reconstruction surgeries.
Advantages of Upper Jaw Implants
Upper jaw implants offer numerous benefits compared to removable prostheses or classical bridgework:
Superior Aesthetics & Natural Appearance
Implants help support facial structure and maintain proper lip and cheek position.
Strong Chewing Function
Patients can comfortably chew a wide variety of foods—including harder textures.
Long-Term Durability
With proper care, implants can last 30+ years or even a lifetime.
Prevention of Further Bone Loss
Implants stimulate the bone, preventing resorption that typically occurs with missing teeth.
Improved Speech & Stability
Common issues with removable dentures—slipping, clicking or speech distortion—are eliminated.
Materials & Digital Technologies Used in Upper Jaw Implants
Modern implant systems are made from biocompatible materials such as titanium and zirconia, ensuring excellent tissue compatibility and reduced allergic risk.
Additionally, advanced technologies significantly enhance accuracy:
• 3D guided implant surgery
• Digital smile design (DSD)
• CAD/CAM-milled implant prosthetics
• CBCT-based surgical mapping
• Computer-generated implant guides
These innovations minimize surgical risks and maximize the predictability of the final result.
Healing Process After Upper Jaw Implant Placement
The first 48 hours are critical for early healing. Mild swelling or sensitivity is normal and resolves quickly. Following the dentist’s instructions accelerates recovery.
General healing timeline:
• Day 1: Soft foods, no hot meals
• 1 Week: Stitches removed, discomfort largely resolved
• 1–3 Months: Osseointegration completed
• After 3 Months: Permanent crowns or bridges placed
Maintaining high oral hygiene and attending routine check-ups is essential for flawless healing.
Upper Jaw Implant Costs: What Affects Pricing?
The total cost varies from patient to patient due to several factors:
• The implant brand and system used
• Whether sinus lifting or grafting is required
• Number of implants placed
• Need for zygomatic implants
• Use of guided or digital surgery
• Type of prosthetic restoration (zirconia, E-max, hybrid, etc.)
Because preparation and bone regeneration are often more complex in the upper jaw, treatment fees tend to be slightly higher than lower-jaw procedures.
Long-Term Care & Maintenance for Implants
The longevity of implants depends heavily on proper oral hygiene and regular professional follow-up.
Recommended maintenance includes:
• Brushing twice a day with proper technique
• Using interdental brushes and floss
• Water flosser for improved hygiene
• Professional cleaning every 6 months
• Annual implant check-ups
These steps prevent peri-implantitis and preserve implant stability for decades.
Conclusion: Upper Jaw Implants Offer a Stable, Aesthetic and Life-Changing Solution
Despite the anatomical challenges of the maxilla, modern dentistry enables safe, predictable and permanent implant solutions for the upper jaw. With proper planning, advanced digital tools, and an experienced surgical team, patients achieve a natural smile, strong chewing ability and long-term comfort.
Upper jaw implants are one of the most reliable investments for patients seeking a permanent, fixed and aesthetic dental restoration.